
 In
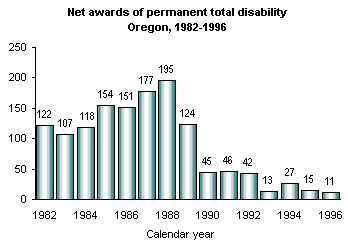
1996, the Oregon workers’ compensation system granted 17
awards of Permanent Total Disability (PTD) benefits and rescinded
six, for a net total of 11 claims awarded PTD benefits.
In
1996, the Oregon workers’ compensation system granted 17
awards of Permanent Total Disability (PTD) benefits and rescinded
six, for a net total of 11 claims awarded PTD benefits.
Declining PTD grants. The figure of 11 net PTD awards in 1996 is a record low. The large drop since 1988 in net PTD awards is primarily the result of the declining number of PTD grants, as there has been no sustained increase in the number of benefit rescissions. In 1988, PTD grants totaled 73 at the Evaluation Unit of the Workers’ Compensation Division and 127 at the Hearings Division of the Workers’ Compensation Board, compared to 1996 figures of 4 and 7, respectively.

Changes to statute and administrative rules have had an effect on PTD grants. The 1987 reforms (House Bill 2900) mandated use, at all levels, of standards for evaluating permanent disabilities. New administrative rules on evaluating disability (OAR 436 chapters 30 and 35), implemented during 1988, provided a more uniform process for claim determination. A later amendment, effective in late 1990, codified case law that had strictly interpreted the statutory mandate that a potential PTD claimant seek regular and gainful employment. Claimants seeking PTD because they are unable to “perform work at a gainful and suitable occupation” must obtain testimony from a certified vocational counselor (see excerpts from Oregon Administrative Rules).
Changes in claims handling are another likely factor behind the decrease in PTD grants, the SAIF Corporation, for example, created a “Critical Claims Unit” focused on management of claims for severe injuries. Medical treatment and rehabilitation may have become more effective in promoting employability and return to work, and there may be more emphasis on those goals due to increased regulation of medical care by the department and to raised ceilings on worksite modification costs and obtained employment purchases.
Perhaps most significant in sustaining the trend of fewer PTD grants has been the claims disposition agreement (CDA, also know as compromise and release settlement), legalized by Senate Bill 1197 in 1990. In a CDA settlement, a worker typically gives up the right to future benefits, except medical services, in exchange for a lump-sum settlement. The nearly 19,000 agreements approved by the Workers’ Compensation Board through fiscal year 1996 certainly include cases that would have been awarded PTD at some level of the system. For example, of the 72 PTD awards rescinded since 1991, 28 had been settled in full (as of July 1997) via a CDA. One implication for grant counts is that 28 claimants will not attempt to obtain reinstatement of their PTD awards. Note, however, that this report does not count a CDA as a rescission of a PTD award.
In sum, there is no single explanation for the decline in PTD grants. Factors having a broad impact upon the workers’ compensation system, such as changes in Oregon’s economy, shifts in the industrial mix away from more hazardous forms of employment, and increased emphasis upon workplace safety and health, may have reduced injury severity, as well as incidence.
Costs. Reports by carriers of their net costs (average cost of grants multiplied by number of net grants) for 1996 PTD cases totaled $7.9 million, compared to $11.9 million in 1995 and about $64.9 million in 1988. These figures represent paid costs for all indemnity awards, medical care, and rehabilitation; plus reserves set aside for future expenses; minus anticipated relief from the Handicapped Workers Program and reimbursements for Preferred Workers; and excluding Retroactive Program benefits.
Following are costs and other claim characteristics for grants awarded in 1996, with comparisons made to 1995 and 1988 grant cases.
 The
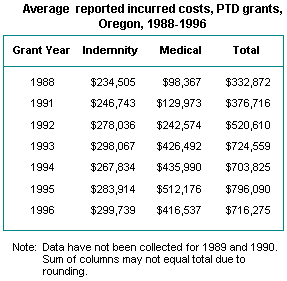
table displays average incurred costs for PTD grants only, rather
than net PTD awards. Average total costs have more than doubled
since 1988, despite a decline of 10 percent in 1996 compared
to the previous year. A small increase in average indemnity was
more than offset by a nearly $100,000 drop in average medical
costs, but the small number of claims also contributes to volatility
in average costs. Average medical costs, though decreasing in
1996, remain more than four times what they were in 1988, due
to the increasing cost of medical care within the system in general,
and the likelihood that claims granted PTD represent injuries
more severe than in the past.
The
table displays average incurred costs for PTD grants only, rather
than net PTD awards. Average total costs have more than doubled
since 1988, despite a decline of 10 percent in 1996 compared
to the previous year. A small increase in average indemnity was
more than offset by a nearly $100,000 drop in average medical
costs, but the small number of claims also contributes to volatility
in average costs. Average medical costs, though decreasing in
1996, remain more than four times what they were in 1988, due
to the increasing cost of medical care within the system in general,
and the likelihood that claims granted PTD represent injuries
more severe than in the past.
The incurred costs for the PTD award make up a large portion of incurred indemnity, which may also include temporary and permanent partial disability, and rehabilitation. Factors influencing trends in PTD indemnity costs include the benefit schedule in effect for the date of injury and the worker’s weekly wage and life expectancy. For all but two 1996 grants, PTD indemnity benefits were calculated at two-thirds of the injured worker’s wage up to a maximum benefit limitation equal to the statewide average weekly wage in effect at the time of the injury (plus allowances for dependents, minus offset for Social Security benefits). On the average, workers granted PTD benefits during the last two years were earning about 109 percent of the statewide average weekly wage used in calculating benefits. For the last three years, around 80 percent of grants have received less than the benefit maximum, compared to 75 percent of the 1988 grants.
The relative stagnation in average incurred indemnity has occurred despite benefit maximums that have increased annually, and indications of more expense from the factor of life expectancy as measured by the declining average age at the time of injury. The average age of claimants at the date of injury has been in the 45-to-46-year range since 1992, compared to about 49 years for 1988 grants.
Insurers. In 1996, SAIF was the insurer in 47.1 percent of the PTD grants, compared to 43.8 percent the previous year. Private carriers covered 35.3 percent and self-insurers, 17.6 percent. One claimant worked for an employer with assigned-risk coverage. In 1988, SAIF carried 61.1 percent of PTD grant cases.
For 1996 grants, the average lag from date of injury to date of order granting PTD benefits increased to 8.7 years, compared to 6.5 for the last two years.
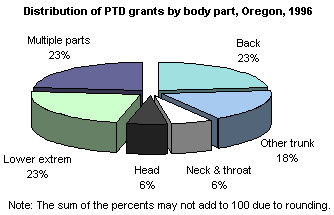 Body part. In 1996, PTD grants involved
injuries to the back in 23 percent of the cases. In 1995, the
back was the injured body part in 22 percent of the cases, while
in 1988, the back was involved in 57 percent of grants. Over
the last 15 years, back injuries as a percentage of all accepted
disabling claims reached a peak (31 percent) in 1986, declining
thereafter until reaching figures currently in the range of 27
to 29 percent. The change in back injuries as a percentage of
all accepted disabling claims does not, by itself, explain the
steep drop in back injuries leading to PTD awards.
Body part. In 1996, PTD grants involved
injuries to the back in 23 percent of the cases. In 1995, the
back was the injured body part in 22 percent of the cases, while
in 1988, the back was involved in 57 percent of grants. Over
the last 15 years, back injuries as a percentage of all accepted
disabling claims reached a peak (31 percent) in 1986, declining
thereafter until reaching figures currently in the range of 27
to 29 percent. The change in back injuries as a percentage of
all accepted disabling claims does not, by itself, explain the
steep drop in back injuries leading to PTD awards.
Other claims characteristics. The small number of grant cases in recent years warrants caution in identifying trends in other claims characteristics. In 1996, manufacturing led all other industries with 6 PTD grants, but no occupational group stood out from the others.
For 1996 grants, the worker had been with the employer an average of just under five years when the injury or illness occurred, similar to figures for 1995 and 1988 cases. Men accounted for not quite two-thirds of PTD claimants in 1996, compared to over 80 percent the previous year.
For grants since 1992, injuries to muscles and tendons (includes sprains and strains) have been the most prominent nature of injury, accounting for 31 percent of cases. The event most often resulting in a PTD grant has been a fall, at 28 percent of cases. Structures and surfaces have been the most frequent source of injury leading to PTD, at 26 percent
Excerpts from Oregon Administrative Rules on
Permanent Total Disability, Effective 2/17/96
Determining Permanent Total Disability
436-030-0055 (1) A worker is permanently and totally disabled if permanently incapacitated from regularly performing work in a suitable and gainful occupation. For the purpose of this rule:
(a) “Incapacitated” from regularly performing work means that the worker does not have the necessary physical and mental capacity and the work skills to perform work.
(b) “Suitable occupation” means those occupations that exist in a theoretically normal labor market, within a reasonable geographic distance, for which a worker has the training or experience, and abilities to realistically perform the job duties, with or without rehabilitation.
(c) “Gainful occupation” is defined as: those types of general occupations that pay wages equivalent to, or greater than, the state mandated hourly minimum wage. Those types of general occupations that pay on a commission or piece-work basis, as opposed to a wage or salary basis, may not be “gainful employment” depending upon the facts of the individual situation.
(d) “Work skills” as used in this rule means: those skills acquired through experience or training that are necessary to gain and adequately perform skilled, semi-skilled or unskilled occupations. Unskilled types of general occupations require no specific skills that would be acquired through experience or training to be able to gain and adequately perform the unskilled occupation. Every worker has the necessary work skills to gain and adequately perform unskilled types of general occupations with a reasonable period of orientation.
(e) A “reasonable geographic distance” as used in this rule means either of the following unless the worker is medically precluded from commuting:
(A) The area within a 60-mile radius of claimant’s place of residence at the time of:(i) the original injury; or
(ii) claimant’s last gainful employment; or
(iii) determination by the department; or
(iv) reconsideration by the Appellate Unit.(B) The area in which a reasonable and prudent uninjured and unemployed person, possessing the same physical capacities, mental capacities, work skills and financial obligations as claimant does at the time of his rating of disability, would go to seek work.
(f) “Types of general occupations” as used in this rule means: groups of jobs which exist in a theoretically normal labor market, and share similar vocational purpose, skills, duties, physical circumstances, goals, and mental aptitudes. It does not refer to any specific job or place of employment for which a job or job opening currently exists.
(g) “Theoretically normal labor market” as used in OAR 436-030-0055 and 0065 means a labor market that is undistorted by such factors as local business booms and slumps or extremes of the normal cycle of economic activity or technology trends in the long-term labor market.
(2) Disability which existed before the injury shall be included
in determining permanent total disability.
(3) In order for a worker to be determined permanently and totally
disabled, a worker must:
(a) prove permanent and total disability;
(b) make reasonable effort to find work at a suitable and gainful occupation or actively participate in a vocational assistance program, unless medical or vocational findings, including the residuals of the compensable injury, make such efforts futile; and
(c) be willing to seek regular and gainful employment.
(4) When a worker retains some residual functional capacity
and is not medically permanently and totally disabled, the worker
must prove inability to regularly perform work at a gainful and
suitable occupation, and the futility of seeking work if claimant
has not made reasonable work search efforts, by competent written
vocational testimony. Competent written vocational testimony
is that which is available at the time of closure or reconsideration
and comes from the opinions of persons fully certified by the
State of Oregon to render vocational services. It does not include
opinions by claimants, physicians or others not certified.
(5) Every Determination Order which grants permanent total disability
shall notify the worker that:
(a) The claim shall be reexamined by the insurer at least once every two years, and may be reviewed more often if the insurer chooses.
(b) The insurer may require the worker to provide a sworn statement of the worker’s gross annual income for the preceding year. The worker shall make the statement on a form provided by the insurer in accordance with the requirements under section (6) of this rule.
| DCBS Public Home Page | IMD Home Page | Site Search Engine |
If you have questions about the information contained in this
document please contact by e-mail or phone:
Mike Maier, Research
Analyst, Research & Analysis Section, Information Management
Division (503) 947-7352.
This document was originally published in October 1997.
Document URL: http://www.cbs.state.or.us/external/imd/rasums/6_2112s.htm
[Printed form: 440-2112(9/97/IMD)]
In compliance with the Americans with Disabilities Act (ADA),
this publication is available in alternative formats by calling
(503) 378-8254 (V/TTY).
The information in IMD publications is in the public domain and
may be reprinted without permission.