
Introduction
Introduction
Under Oregon workers’ compensation law, injured workers, insurers, and medical providers may request resolution of medical disputes by the director of the Department of Consumer & Business Services (the department). Parties may request review of disputes involving medical services and treatments, palliative care, fees, changes of attending physician, and requests for additional insurer medical exams (IMEs). Statutory authority to resolve medical disputes is given to the director under Oregon Revised Statutes (ORS) 656.245, 656.248, 656.260, 656.325, and 656.327. Oregon Administrative Rules (OAR) Chapter 436, Divisions 9 and 10, provide the guidelines for administering the delivery of and payment for medical services and for resolving disputes.
The WCD Medical Review and Abuse Section was created in February 1990 to handle medical disputes. In 1992, during a WCD reorganization, the section was reorganized and renamed the Medical Review Unit (MRU). At that time, the WCD Benefits Section assumed responsibility for resolving two issues: changes of attending physician and requests for additional IMEs. Effective October 23, 1999, Senate Bill 728 transferred responsibility for disputes when compensability of the underlying medical condition is at issue to the Workers’ Compensation Board Hearings Division. (The results of this change are outside the time frame of this report.)
This report presents information about medical dispute activity for fiscal year 1999. The data include disputes received and resolved, disputes involving managed care organizations, the time required to process requests, and appeals of the orders. Additional information is available from the department’s Research & Analysis Section.
Highlights of the Report
In FY99, the department received 862 medical dispute requests. Of these, 62 percent were medical service disputes, 24 percent were treatment disputes, and 5 percent were palliative care disputes.
In FY99, 825 medical disputes were resolved. Of these disputes, 54 percent were approved, 23 percent were disapproved, and 6 percent were partially approved. Two percent of the resolutions were stipulations. Fourteen percent of the disputes were dismissed or withdrawn.
Nineteen percent of the FY99 orders resolved disputes that involved managed care organizations. Forty-seven percent were medical service disputes, 47 percent were treatment disputes, and 6 percent were palliative care disputes.
In FY99, the average number of calendar days from the receipt of a dispute to its resolution was 105 days. There is great variability in the resolution time of different issues. Treatment disputes averaged 160 days to resolve, while IME disputes averaged 37 days. Nearly 80 percent of the treatment disputes that were resolved required the use of outside physician reviewers. This review added an average of 24 days to the processing time.
Fourteen percent of the FY99 orders were appealed to contested case hearings.
Legislative history
Most legislative sessions since 1987 have produced changes in the medical dispute resolution process. In 1987, House Bill 2900 allowed the director to establish a medical review panel to review, upon request of any of the parties, the medical treatment of an injured worker. This review process was seldom used. HB 2900 also limited IMEs to three per each opening of the claim, unless authorized by the director.
The administrative dispute resolution process became mandatory for medical disputes when Senate Bill 1197 took effect July 1, 1990. In part, the intent of SB 1197 was to reduce litigation by placing the responsibility for medical decisions on the department’s medical personnel. SB 1197 also eliminated most palliative care after the worker becomes medically stationary; this eliminated many potential disputes.
Following the Court of Appeal’s decision in Meyers v. Darigold in October 1993, the director lost jurisdiction over disputes involving proposed medical treatment. SB 369, effective June 7, 1995, restored this jurisdiction to the director. SB 369 also allowed a worker (not just the worker’s attending physician) to request approval for palliative care when the insurer denies the care. Also, SB 369 took jurisdiction for appeals of medical dispute orders, other than orders concerning additional IMEs, from the Workers’ Compensation Board Hearings Division. These disputes are now heard as “contested cases.”
The 1999 legislative session produced two changes. HB 2525, effective August 1, 1999, moved the contested cases hearings officers (who hear most appeals of medical dispute orders) from the department to the Oregon Employment Department. Effective October 23, 1999, SB 728 transferred responsibility to the Hearings Division for disputes when compensability of the underlying medical condition is at issue or when the causal relationship between the accepted condition and the medical service is at issue.
Medical disputes received
In fiscal year 1999, the department received 862 requests for medical dispute resolution (see Table 1). This was a 3 percent increase from the number in FY98. Sixty percent of the requests were from workers or their attorneys, 28 percent were from medical providers, and 10 percent were from insurers.
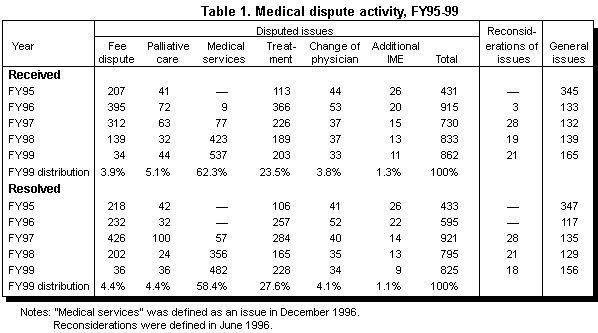
The most common type of medical dispute is over medical services. These disputes are about the services, other than palliative care, to which a worker is entitled. In FY99, 62 percent of the disputes fell into this category. This category was created in December 1996 when the coding system was revised to better match the medical service sections of the statute. (Compensable medical services are defined in ORS 656.245.) Many issues formerly defined as palliative care or fee disputes are now classified as medical service disputes. Palliative care disputes arise when a worker or the worker’s attending physician requests that the insurer approve palliative care to enable the worker to continue current employment after the worker has become medically stationary. Claimants and providers bring these disputes to the department. Fee disputes are disputes between an insurer and medical provider regarding the amount of a fee for a medical service. Often, the medical provider requests reimbursement on a reduced bill. These two types of disputes accounted for 9 percent of the disputes.
Treatment disputes are the other common category of dispute. Treatment disputes are those in which a worker or an insurer claims that the medical provider’s treatment is inappropriate, excessive, ineffectual, or in violation of the administrative rules. Nearly a quarter of the disputes received in FY99 were treatment disputes. Over three-quarters of the insurer requests involved treatment issues. As will be shown later, treatment disputes are the most contentious and difficult to resolve.
Change of physician disputes occur when a worker requests an additional change of attending physician beyond the two changes allowed by statute. Insurer medical exam disputes arise when an insurer requests that a worker undergo an additional medical exam beyond the three allowed in statute. These two categories accounted for 5 percent of the FY99 disputes.
In addition to these disputes, there are also reconsiderations and general issues. Reconsiderations are cases in which the department reconsiders its own order. The parties may request reconsideration of an order within 30 days if they believe the order contains errors or misapplications of the law or if they have new evidence that could not reasonably have been discovered or produced during the review. There were 21 reconsideration requests in FY99. They were nearly evenly split between medical service and treatment issues.
General information requests are requests of a general nature. They are not considered disputes, and they do not require a director’s order to resolve. Rather, informational letters are used to respond to these requests. More than 160 of these general requests were received in FY99.
Dispute orders
During FY99, 825 disputes were resolved. Of these orders, 14 percent were orders of dismissal (see Table 2a). A dismissal may occur for a variety of reasons, such as the inappropriate, incomplete, or untimely submission of the request or because the request was withdrawn. There were far fewer dismissals in FY99 than in FY98, when 45 percent of the requests were dismissed. The decline resulted from a change in MRU’s procedures. In the past, if the insurer agreed to pay during the processing of a dispute, MRU issued a dismissal order. In FY99, MRU issued approval orders in these situations.
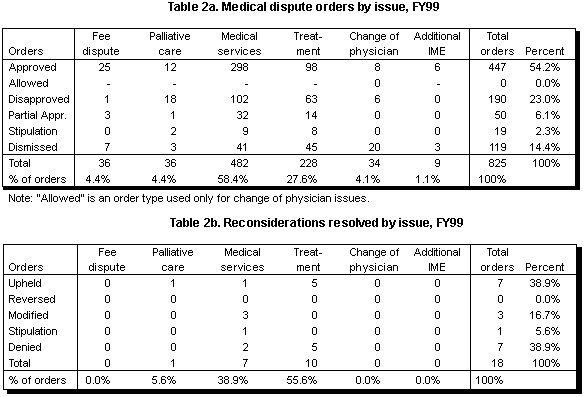
Fifty-four percent of the FY99 orders were orders of approval, 23 percent were disapproval orders, and 6 percent were partial approvals. Approval orders are those that order payment to providers, approve palliative care, approve all of the medical provider’s treatment, or approve the additional change of attending physician or additional IME. Denial orders deny these items. Partial approval orders are orders that approve part, but not all, of the request for additional reimbursement, palliative care, or treatment.
Two percent of the FY99 orders were resolved by stipulation. Stipulations are written agreements between the disputing parties that are reached through mediation.
There is one other possible outcome: “allowed.” This outcome allows the change of physician when the statutory limitation on the number of changes has not been exceeded. There were no orders of this type in FY99.
Excluding the dismissed cases, 68 percent of the disputed medical services were approved, 23 percent were disapproved, and 9 percent were settled with a partial acceptance or a stipulation. Again excluding the dismissed cases, 54 percent of the disputed treatments were approved, and 34 percent were disapproved. Less than half of the requests for palliative care were approved. Most of the requests for payment of disputed billings were approved.
Medical providers were usually successful when they requested dispute resolution. Excluding the dismissals, over 80 percent of the medical services for which providers requested approval were granted.
When it reconsidered its earlier orders, MRU seldom changed its previous decision (see Table 2b). In 14 of the 18 cases, the reconsideration was denied or the earlier order was upheld.
Disputes involving managed
care organizations
In FY99, 19 percent of the orders resolving disputed issues involved managed care organizations. MCOs must have internal dispute resolution processes, although they may choose to have the department resolve certain types of issues. Therefore, medical disputes come to the department either because the MCO does not have a resolution process for a particular type of dispute or because the MCO’s decision is being appealed. About 40 percent of the workers with accepted disabling claims are enrolled in MCOs. The small number of MCO disputes received by the department indicates that the MCOs resolved many medical disputes.
The disputed issues involving MCOs were nearly evenly split between medical service and treatment disputes (see Table 3). Thirty-two percent of all orders resolving treatment disputes involved MCOs. In comparison, 15 percent of the medical service disputes involved MCOs. This difference may indicate that MCOs had more difficulty resolving treatment disputes internally than medical service disputes.
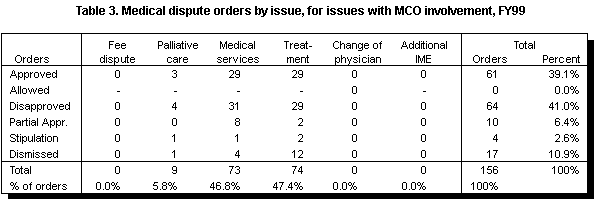
For the disputes involving MCOs, the department issued approximately equal numbers of approval orders and disapproval orders. This contrasts with the disputes that did not involve MCOs; in this group, there were more than three times as many approval orders as disapproval orders.
Processing times
The average number of calendar days from the initial receipt of a dispute to its resolution was 105 days for FY99 orders (see Table 4). This compares to 101 days in FY98. Treatment disputes took the longest to resolve, 160 days. Palliative care disputes averaged 137 days. IME disputes were resolved the most quickly, averaging 37 days.
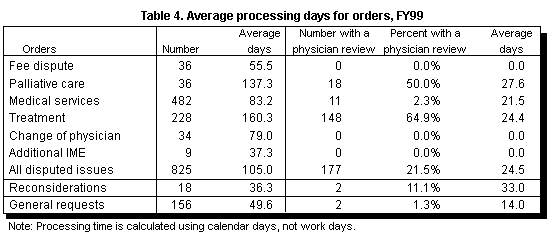
A portion of this processing time can be attributed to the involvement of outside physician reviewers. These reviewers or panels of reviewers may be appointed by the department to review the disputed treatments, medical services, or palliative care. Sixty-five percent of the treatment orders (nearly 80 percent of the treatment orders that were not dismissed) utilized outside physician review. The length of time from the date of the department’s letter establishing the outside review to the date that the physician’s report was received averaged 25 days.
Appeals of orders
Orders from disputed issues other than IMEs can be appealed through the contested case hearings process. (IME orders are appealed to the Hearings Division.) Prior to August 1, 1999, these hearings officers were under the director’s jurisdiction. They have become a part of a centralized hearings panel in the Oregon Employment Department. Parties have 30 days to appeal a medical dispute order.
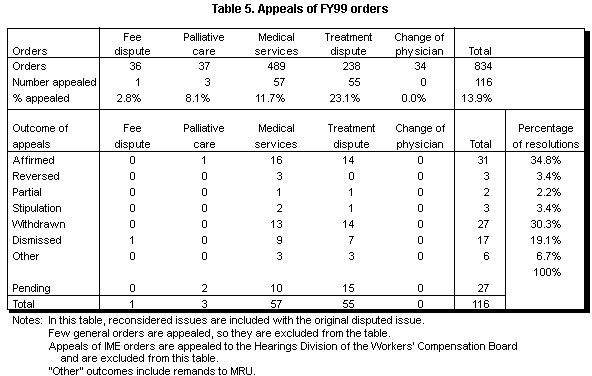
Of the orders issued in FY99, 14 percent were appealed (see Table 5). Twenty-three percent of the treatment dispute orders were appealed. As of January 2000, 77 percent of the appealed orders had been resolved. Nearly half of the appeals were either withdrawn or dismissed. Most of the decisions were affirmations of the earlier order.
DCBS Public
Home Page | IMD
Home| IMD
Search |
If you have questions about the information contained in this document please contact by e-mail or phone: Gary Helmer, Research Analyst, Research & Analysis Section, Information Management Division (503) 947-7325.
This web page was last revised: 04/11/00.
In compliance with the Americans with Disabilities Act (ADA), all IMD publications are available in alternative formats by calling (503) 378-4100 (V/TTY). The information in IMD publications is in the public domain and may be reprinted without permission.
[Printed form 440-2407(4/00/IMD)]