
Oregon law (ORS 656.273) sets a five-year limit in which a worker is entitled to additional benefits when aggravation of a compensable injury or illness occurs. Beyond this aggravation period, workers must petition their insurer or the Workers’ Compensation Board in order to reopen a claim. Upon its own motion, the board may grant temporary total disability (TTD) benefits in these cases. According to (ORS 656.278), the Workers’ Compensation Board retains the authority to modify, change, or terminate former findings, orders or awards. Effective January 1, 1988, House Bill 2900 restricted the board’s own motion authority to cases fulfilling either of the following conditions: (1) post-aggravation-period claims with worsening of a compensable injury requiring hospitalization or surgery or (2) necessary medical services on compensable claims with an injury date prior to 1966.
The reform legislation also established the Reopened Claims Reserve to reimburse insurers or self-insurers for compensation paid to injured workers under own motion action, creating an incentive for carriers to seek an own motion order. Effective 1/1/96, the Reopened Claims Reserve was renamed the Reopened Claims Program (RCP) and became a component of the newly created Workers’ Benefit Fund. While insurers have the authority to voluntarily reopen a claim, the board’s own motion authority is employed when the carrier denies a request for reopening. If the board authorizes a reopening, the insurer is ordered to pay benefits and is reimbursed from the RCP as applicable.
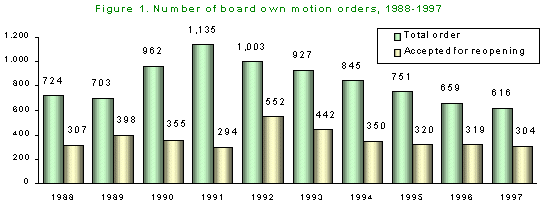
Figure 1 depicts the number of board own motion (BOM) orders from 1988-97. These data are yearly totals of final orders, including claims accepted for reopening, claims denied, and dismissals. In 1997, the board issued 616 orders, continuing a declining trend of total orders since 1991. At a slower rate, the number of claims accepted for reopening has also been decreasing. Reopened claims totaled 304 in 1997, 49 percent of total orders. The decrease in orders and reopened claims is partially related to a period of unusually high activity from 1991-1993, when SAIF began requesting reimbursement from the board on medical services for pre-1966 injuries. Another factor affecting the trend is the 36 percent decline in all accepted disabling claims (ADC) since 1988 (although BOM orders are only affected by claims that are beyond the five-year aggravation period). This abatement in the number of ADC’s is attributed both to increased attention to workplace safety and health, and policy modifications which have resulted in more conservative methods of evaluating claims and compensability.
Reopened Claims Program. The RCP is funded by assessments paid by employers and workers; these costs are excluded from the premium base. As of May 1998, RCP reimbursements to insurers and self-insurers total $33 million on BOM cases with order dates of 1988-1997. Reimbursements on a cash-flow basis were $3.6 million in FY 1997, a 24 percent increase from the 1996 total. The four-year average on a cash-flow basis is now $3.4 million per year.
The data reported herein include only reopened claims where insurers and self-insurers have been reimbursed; some BOM orders exist where the carrier has not requested RCP reimbursement. Unless otherwise noted, statistics are based on the most recent BOM order date affecting the case (interim order date), which is not necessarily the date the board first ordered the claim reopened. Thus, yearly totals of orders and reimbursements may fluctuate whenever the board amends an order.
Reimbursed medical claims. As Figure 2 shows, 7 own motion orders in 1997 were claims for medical services. This continues a downward trend since 1992, when order activity peaked, as mentioned earlier, due to SAIF’s reimbursement requests. With some costs still outstanding, the average reimbursement per medical claim was $13,169 as of May 1998, compared to the average of $16,995 for medical services on 13 BOM orders in 1996. Total reimbursements for medical services on 1997 orders stand at $92,184, compared to the high of $3.2 million for 1992 orders.
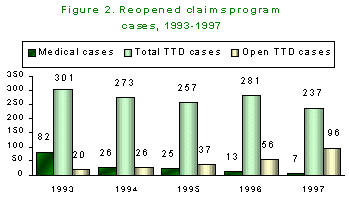
Reimbursed temporary total disability claims. Claims with RCP reimbursements for TTD decreased to 237 for 1997 BOM orders. As of May 1998, TTD reimbursements accounted for 94 percent of total reimbursements on 1997 orders, roughly comparable to the percentages of previous years (excluding 1992 and 1993 when reimbursements for medical services were anomalously high). The largest reimbursement for a post-aggravation TTD case closed in 1997 was $205,121. For TTD cases closed in 1997, the median reimbursement was $3,718, the highest figure since 1994, and the median time lag from date of BOM order to insurer closure was 7.8 months.
On claims reimbursed under a 1997 BOM order, the median time lag from date of injury to date of order was 10.7 years; the average time lag was 12.3 years (the difference in figures due to some claims with lengthy time lags, the longest being 35 years). Broken down by type of insurer, SAIF was reimbursed in 50 percent of the 1997 TTD cases, a rate similar to those in previous years. Private insurers comprised 31 percent of the reimbursed cases in 1997, while self-insurers made up 19 percent.
Reopened TTD claim characteristics. Although these data describing characteristics of reopened TTD claims pertain to the original injury or illness rather than the circumstances of the aggravation, they may nonetheless shed some light on the types of cases that require reopening beyond the aggravation period.
For 1997 orders, the average age at the date of original injury was 34, equaling the average age of 34 for the last three years. This along with the median time lag from injury date to order date indicates the worsened condition typically flared up when the worker was about 45 years of age.
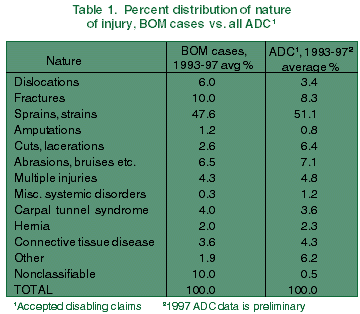
As in previous years, sprains and strains were the most common nature of the original injury in 1997 cases, with 48 percent of the total. Categories with increases from previous years were dislocations, fractures, multiple injuries, and carpal tunnel syndrome, representing 7.2, 11, 5.9, and 8 percent of the 1997 cases, respectively. As depicted in Table 1, the average distribution of sprains and strains for reopened claims is slightly less than that of all accepted disabling claims, suggesting this condition is less likely to cause long-term or chronic problems. These data also suggest that dislocations, fractures, amputations, and carpal tunnel syndrome, although less probable as original injuries, are more likely to lead to long-term medical problems.
The most common source
of the original injury was structures and surfaces (20 percent),
and the causal event with the highest frequency was overexertion
(30 percent). Figure 3 shows the percent 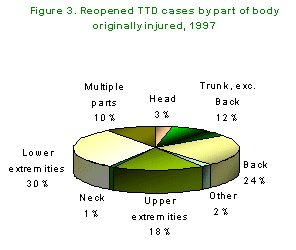 distribution
of the body part originally injured in 1997 cases. Since 1991,
BOM cases have reported the lower extremities as the part most
frequently injured; the five-year average of 34 percent is substantially
higher than the 20 percent occurrence among all accepted disabling
claims.
distribution
of the body part originally injured in 1997 cases. Since 1991,
BOM cases have reported the lower extremities as the part most
frequently injured; the five-year average of 34 percent is substantially
higher than the 20 percent occurrence among all accepted disabling
claims.
For 1997 orders, the
industry with the highest percentage of claimants was manufacturing
(36 percent). Operators (excluding transportation operators)
comprised the most common occupation group, with 16 percent of
the total. Twenty-nine percent of claimants were female, a figure
higher than the 1992-96 average of 23 percent. Median length
of employment with the employer at the time of injury was 1.5
years. Finally, at the time of the original injury, the weekly
wage earned by workers with a 1997 Board Own Motion claim averaged
8 percent higher than the statewide weekly wage.
If you have questions about the information
contained in this document please contact by e-mail or
phone: Charles Forbes,
Research Analyst, Research & Analysis, Information Management
Division
(503)947-7329 .
This document was originally published in September 1998.
Printed form: 440-2425 (09/98/IMD)
Document URL: http://www.cbs.state.or.us/external/imd/rasums/7_2425s.html
In compliance with the Americans with Disabilities Act (ADA),
this publication is available in
alternative formats by calling (503) 378-4100 (V/TTY).
The information in IMD publications is in the public domain and
may be reprinted without permission.