
Introduction
The Workers’ Compensation Division of the Department of Consumer
and Business Services (DCBS) investigates allegations of statute or administrative
rule violations in an effort to minimize abuse of the workers’ compensation
system. The division investigates complaints involving abuse or fraud
by medical providers, insurers, employers, and claimants. This report
summarizes the division’s complaint investigation activity from July
1, 1999 through June 30, 2000 (FY00).
Investigations opened
In FY00, 253 investigations into complaints of abuse or fraud were opened
averaging 21 a month. This is a 9.5 percent increase from the 231 investigations
opened in FY99. Until FY98 the number of investigations opened had been
decreasing every year since FY 93, when a high of 342 investigations were
opened. The increased investigations in FY00 continues an upward trend
of investigations opened beginning in FY98.
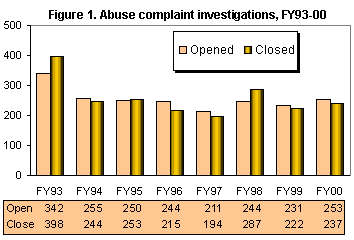
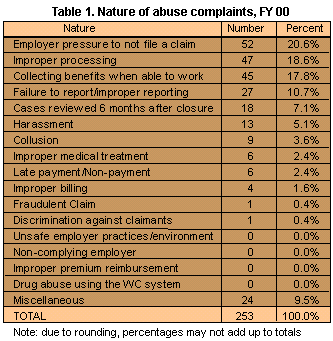
Table 1 shows the nature and number of abuse complaints for FY00. The most frequent complaints received were for employer pressure to not file a claim (52 or 21 percent of the total), improper processing (47 or 19 percent of the total), collecting workers’ compensation benefits when able to work (45 or 18 percent of the total). Other complaints included: failure or improper reporting of claims-related documents by either the employer, insurer, or medical provider (27 or 11 percent of the total), harassment (13 or 5 percent of the total), and improper billing (4 or 2 percent of the total). All other complaints accounted for 24 percent of the total investigations opened (including 18 cases reviewed 6 months after closure).
Subject of investigations opened
Twenty-one percent (53) of the 253 complaint investigations opened in
FY00 were against workers. Of these investigations, 77 percent (41) were
for collecting workers’ compensation benefits when able to work.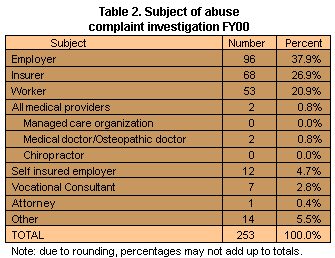
Thirty-eight percent (96) of the investigations were against employers. This is an increase from FY99 where 35 percent (82) of the investigations opened were against employers. Forty-nine percent (47) of the investigations against employers were for employer pressure to not file a claim. Twenty-seven percent (68) of the investigations were against insurers; 44 percent of those investigations were for improper claims processing. All medical providers accounted for one percent (2) of the investigations and self-insured employers accounted for five percent (12) of investigations opened.
Investigations closed
In FY00, 237 investigations of abuse or fraud complaints were closed compared
to 222 closures in FY99. An average of 20 complaint investigations were
closed each month in FY00. These complaints were closed either by disposition
(61 percent) or by referral (39 percent). Of the 144 disposed complaints,
69 (48 percent) were unfounded, 26 (18 percent) were retained for pattern
development, 24 (17 percent) were issued a letter of reprimand or warning,
and 20 (14 percent) were given a letter of notification.
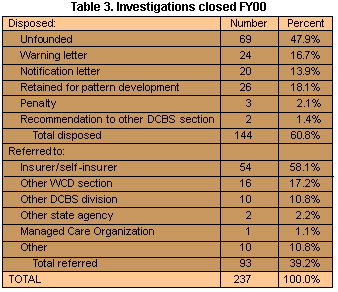 Thirty-nine
percent (93) of the investigations were closed by referral. Fifty-eight
(54)percent of these referrals were made to the insurer (or self-insurer).
Complaints referred to the insurer most often consisted of claimant fraud
such as collecting workers’
Thirty-nine
percent (93) of the investigations were closed by referral. Fifty-eight
(54)percent of these referrals were made to the insurer (or self-insurer).
Complaints referred to the insurer most often consisted of claimant fraud
such as collecting workers’
compensation benefits when able to work (76 percent). Seventeen percent
(16) of the referrals were to another WCD section, eleven percent (10)
were made to another DCBS division and two percent (2) were made to another
state agency.
If you have questions about the information contained
in this document please contact by e-mail or phone: Ed
Bissell Research Manager, Research & Analysis Section, Information
Management Division (503) 947-7364. This document was originally published
in May 2001.
[Printed form: 440-2471(05/01/imd)]
In compliance with the Americans with Disabilities Act (ADA), this publication is available in alternative formats by calling (503) 378-4100 (V/TTY). The information in IMD publications is in the public domain and may be reprinted without permission.